This is your service connection 101 guide. An overview of how veterans can establish service-connection for VA disability compensation.
There are several different ways to get service-connected. Below, we’ll go through each of the six main methods.
Direct Service Connection
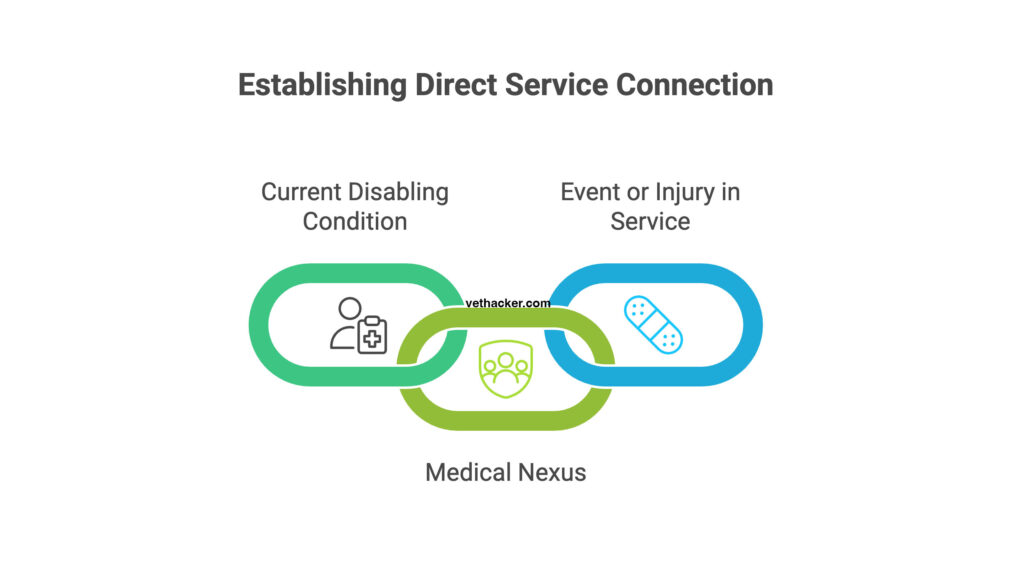
This is the most common type of service connection and the one most veterans are familiar with.
To establish direct service connection, you must prove three things:
- You have a current disabling condition
- There was an event, injury, or disease during service
- There is a medical nexus linking the current disability to that in-service event or injury
It sounds simple, but each element has its own requirements.
Evidence of a current disabling condition
This is most commonly established by a medical diagnosis provided by a medical professional. It can’t be based on a lay statement alone. It doesn’t matter how many supporting lay statements you provide or even if you provide a photograph as proof that you have a current disability. It must first be diagnosed by a medical professional.
Exceptions
There are a few exceptions, but they are narrow and specific:
- Undiagnosed Gulf War Illness:
A medical professional must certify that all other diagnoses have been ruled out, and that your condition qualifies as an undiagnosed illness. - Pain causing functional impairment:
The Veterans Court (CAVC) has ruled that if pain causes functional impairment that affects earning capacity, it can qualify as a disability even if it doesn’t meet criteria for a formal diagnosis.
Example:
During a VA examination, a Veteran reports knee pain while running or during prolonged standing. The medical examination reveals no abnormality or weakness or limitation of motion. All imaging, such as x-rays, show normal results. The examiner notes functional limitations, such as inability to stand after a few minutes, significant pain when walking up stairs, and also notes use of a brace and a cane.
The examiner then states that the diagnosis is “subjective knee pain” unsupported by objective testing. The examiner notes that the veteran misses work during flare-up of pain, and is potentially at risk of losing his job because his job requirements involve prolonged standing. In this case, even though there is no diagnosis, the VA may consider the knee pain as evidence of a current disability, since it is shown to result in an impairment of earning capacity.
Evidence of an Event or Injury in Service
In many cases, this is established by an entry in your Service Treatment Record (STR) or military personnel records.
In some instances, you won’t have any documentation in your records of an injury or event in service. However, the lack of specific documentation does NOT automatically mean you don’t meet this criteria.
You can still establish this criteria through:
- Lay statements describing how the injury or event occurred
- Buddy statements or witness statements
What is important to note here is that this is a factual determination to be made by the VA rater.
VA cannot just deny your claim and say that there is no event or injury in service, all because your Service Treatment Records do not show any complaints in service.
If you submit a lay statement, VA must make a determination if the statement that you submitted is competent and credible, and weigh that evidence against your record. Now, it doesn’t mean they have to believe you, it just means that they can’t not believe you outright.
Special cases
- Combat veterans: If you have combat service (typically proven by combat medals), VA must accept your lay statement as evidence – as long as it’s consistent with the circumstances of combat.
- Injuries that normally require treatment: For example, a broken foot is something that would almost always be documented, it’s not one of those things where you just “suck it up” and don’t go to medical. If your STRs show no record of it, the VA may find your lay statement less credible.
Medical nexus
This refers to a medical opinion made by a medical professional, providing a link (or nexus) between your current disability and the event or injury in service.
Now, no two nexus opinions are going to be alike. But, you need two things here:
- It must be specific to you and your case
- It must contain a sufficient medical rationale
What do these mean?
It must be specific to you and your case
This means the medical professional providing the nexus must specifically discuss the specifics of your case. It isn’t enough to say “I found this study that shows that most veterans are predisposed to these kinds of diseases or injuries because of what they go through during deployment. This veteran did not have this disease prior to service and now he has it.”. That’s not going to fly. The opinion must discuss how the study applies to your specific circumstances and must contain a sufficient rationale, as described below.
And, this must be provided by a medical professional. Attorneys or Veterans Service Organizations (VSO’s) trying to provide nexus statements are not acceptable. Simply providing a copy of a medical journal or medical research, then quoting a bunch of laws and then concluding that VA must therefore award service-connection does not meet this criteria under any circumstance, unless the Attorney or VSO is also a medical professional.
It must contain sufficient medical rationale
VA defines an acceptable medical opinion as “a conclusion supported by evidence, including current medical literature as well as examination and evidence in the claims file”
In determining whether a medical opinion has a valid rationale, VA will consider:
- If the medical opinion includes the reasons and basis for the opinion
- Supports conclusions with an analysis that can be considered and weighed against contrary opinions
- Provides not only clear conclusions with supporting data but also a reasoned medical explanation connecting the two.
- A medical opinion is not entitled to any weight if it contains only data and conclusions.
Read that last bullet again. It’s one of the most common mistakes found in medical nexus evidence submitted by veterans. If you’re wondering why VA keeps rejecting the medical nexus from your private doctor vs the opinion from the VA medical examiner, this is the most common reason. Your private doctor must provide a valid rationale, and not just data and conclusions.
Secondary Service Connection
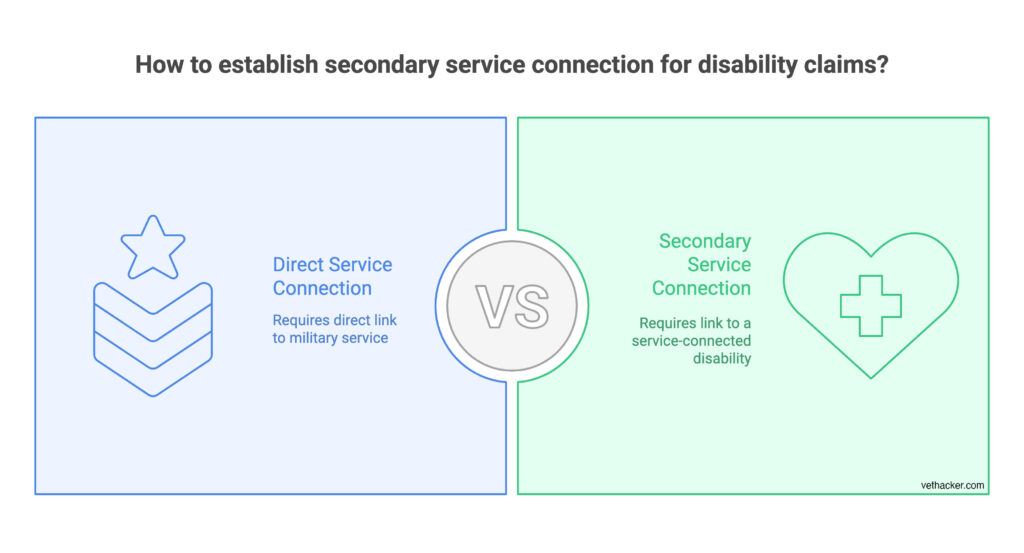
Secondary service connection is granted when a veteran’s current disability, while not directly caused by military service itself, is proximately due to or the result of a service-connected disability they already have.
Similarly, you need to show three things for a claim to be successful:
- Evidence of a current disability
- An already service-connected disability or disease (this is called the primary service-connected disability)
- A medical nexus showing that the current disability (the secondary disability) is caused by the already service-connected disability or disease (the primary disability).
Evidence of a current disability is the same as discussed above.
Typically, #3 is the most confusing part here. Service connection on a secondary basis requires a showing of causation. VA’s own manual states that: A showing of causation requires that the secondary disability be shown to be proximately due to, or the result of, a service-connected condition.
This is where it can sometimes get frustrating for veterans. It doesn’t help that VA raters often misapply the standard of proof here. VA raters occasionally make the mistake of requiring a higher standard for service-connection in secondary service-connection cases.
A common denial is when VA rejects a medical opinion showing causation by stating that while the evidence and medical literature supporting the opinion shows correlation, it does not establish causation.
This is problematic in many ways, because what the rater is effectively doing is requiring the veteran to meet a higher evidentiary threshold to establish service-connection on a secondary basis.
As long as the medical opinion has a clear rationale, even if it is based on studies showing correlation, it can establish causation for VA purposes. Make sure the VA isn’t incorrectly denying your claim by requiring a higher evidentiary threshold to grant.
One thing that VA makes clear is that to establish causation, the primary disability need not be service-connected, or even diagnosed, at the time that the secondary condition was incurred.
That means that VA can’t arbitrarily deny a claim just by saying that the secondary condition was first diagnosed prior to the date you were service-connected for the primary disability.
Obesity as an intermediate step
This is one of the most overlooked way to service-connect disabilities such as obstructive sleep apnea.
VA recognizes obesity as an “intermediate step” between a service-connected disability (the primary disability) and a current disability (the secondary disability) that may be service-connected on a secondary basis.
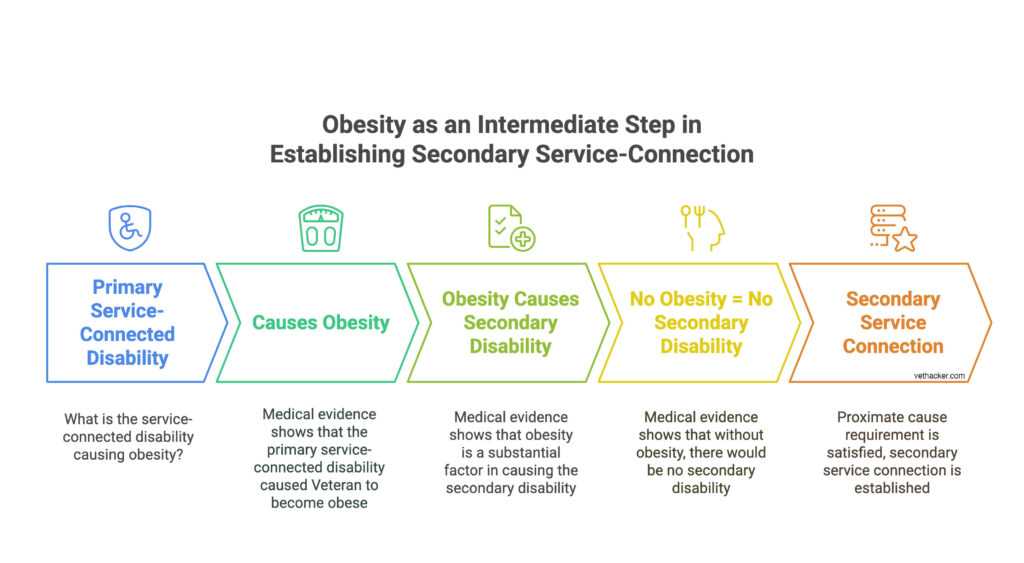
To establish secondary service-connection based on obesity as an intermediate step, the medical evidence must show:
- The primary disability must have caused the veteran to become obese
- That obesity as a result of the primary service connected disability was a substantial factor in causing the secondary disability being claimed
- The claimed secondary disability would not have occurred if the obesity caused by the primary disability was not present
Example: Obesity caused by an orthopedic condition which then leads to obstructive sleep apnea.
Disabilities caused by the effects of medication
This is another overlooked avenue for secondary service-connection. If constant medication because of a primary service-connected condition has resulted in another disability, then that disability can be service-connected on a secondary basis.
Examples:
- Gastroesophageal reflux disease (GERD) that results from long term use of non-steroidal anti-inflammatory drugs (NSAIDs) aka painkillers
- Anemia resulting from cancer treatment
Aggravation of a Nonservice-Connected Disability by a Service-Connected Disability
This is actually a form of secondary service-connection, but there are enough differences under the law that I feel that it’s best to consider it as a “separate” way of service-connection.
Basically, this applies when a service-connected disability worsens (but does not cause) another condition. VA can compensate for the additional level of disability caused by that worsening (aggravation).
To qualify, the evidence must show:
- There must be a measurable increase in the severity of the claimed condition (the secondary nonservice-connected condition).
- The increase in severity must be the result of the primary service-connected disability and not due to natural progression.
- You must establish a baseline severity before aggravation.
The medical evidence must establish the baseline level of severity of the nonservice connected condition. The VA will then only compensate for the degree of disability that is above this baseline and not due to natural progression.
An example here would be kidney disease worsened by, but not caused by service-connected diabetes mellitus. Let’s say a veteran is service-connected for diabetes mellitus, but is not service-connected for hypertension. The medical evidence shows that the kidney disease is caused by long-standing hypertension, and not by diabetes mellitus.
But, diabetes mellitus is known as an accelerating factor for kidney disease. Service-connection can potentially be established for kidney disease if the evidence shows that it was aggravated beyond natural progression by the service-connected diabetes mellitus. But, the evidence must first show a baseline level for the severity of the kidney disease. What VA does is it calculates how much worsening can be attributed to the service-connected diabetes mellitus.
So, in this example, if the baseline evidence shows that the kidney disease would have been rated 30 percent prior to aggravation, but now, symptoms meet the criteria for a 60 percent evaluation after aggravation by diabetes mellitus, VA will deduct the 30 percent baseline from the current 60 percent, and award service-connection for 30 percent.
Presumptive Service Connection
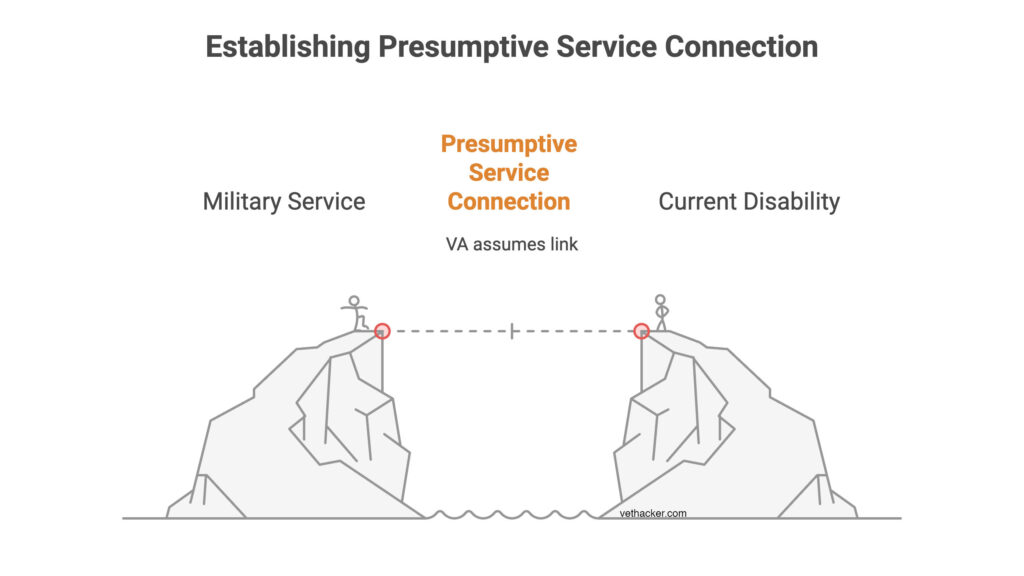
Presumptive service-connection removes the need for a medical nexus between a current disability and service.
Basically, what this means is that VA assumes certain disabilities are service-connected if they meet specific criteria.
For example, if certain chronic disabilities such as hypertension or heart diseases or malignant conditions (cancers) are diagnosed within a year of discharge from service and the severity shows that they meet at least a 10 percent level under the VA’s schedule of rating disabilities, then VA will assume that these disabilities are caused by service, even if they were not shown in your service records or you were never treated for them in service.
There are also times where VA will presume that you were exposed to certain chemicals in service, and in turn, presume that certain disabilities are caused by such exposure.
For example, if you had boots on ground service, even for a day, in the Republic of Vietnam within a certain time period, then VA will presume that you were exposed to herbicides such as Agent Orange. If you are then diagnosed with certain disabilities that are presumptive to herbicide exposure, then you do not need to provide a medical nexus proving that your diagnosed condition is caused by herbicide exposure. The law will fill that in for you and VA will presume that your disability is caused by exposure to Agent Orange.
Another example are the presumptive disabilities associated with Gulf War service or with radiation exposure.
One important thing to keep in mind is that while presumptions simplify the process by “doing the heavy lifting,” you must still have a diagnosis of a current disability. And in some cases, not only must a veteran have a diagnosis, the disability must have symptoms that are severe enough to be rated at a “compensable” level, meaning, if they were to be granted, the symptoms must meet at least the 10 percent disability level.
A common misconception is that simply serving in a presumptive location automatically entitles you to benefits. This is not true. A veteran is not compensated for exposure; they are compensated for a disability presumed to be caused by that exposure. You must have a valid medical diagnosis of a current, diagnosed disability that appears on the VA’s official presumptive list for that specific service era or exposure.
For example, if you served in a location where VA presumes exposure to herbicides such as Agent Orange, and you claim for service-connection for diabetes mellitus, which is a disability that is presumed to be caused by herbicide exposure, but your medical examination shows that you are pre-diabetic, then you won’t be entitled to service-connection. You will be denied for having “no diagnosis”. Being ‘pre-diabetic’ does not qualify as diabetes mellitus for service connection, even if you were exposed to herbicides.
Aggravation of a Pre-service Disability
Also known as pre-service aggravation. Basically, this applies when you had a condition before entering service and claim that service made it worse beyond natural progression.
There are typically two kinds of claim based on aggravation:
- Claims based on the presumption of aggravation – when the disability was noted on your enlistment exam.
- You must prove that the disability noted on enlistment worsened beyond natural progression because of service
- This claim is adjudicated by VA under 38 CFR 38 CFR 3.306
- Claims based on the presumption of soundness – when the disability was NOT noted on your enlistment examination but other evidence indicates that it pre-existed service.
- VA must prove that it existed before service AND that it was not aggravated by service
- If VA cannot prove both, then they must assume that you were sound on enlistment and treat your claim as a claim for direct service connection
- The claim is adjudicated by VA under 38 CFR 3.304(b)
So, basically, the first question to ask is if the disability was noted on your enlistment examination or not.
If it was noted on enlistment (38 CFR 3.306)
If it was noted on your enlistment examination, then the burden is on the veteran to prove that the disability was aggravated beyond natural progression by service.
Under this law, service-connection is granted because the pre-existing disability was aggravated beyond natural progression by service. A claim is denied when the evidence shows that the pre-existing disability was not aggravated beyond natural progression by service.
One of the most common disabilities claimed under this law are flat feet (aka pes planus). Flat feet are typically noted on entry but are typically asymptomatic. If a medical opinion establishes that flat feet were aggravated beyond natural progression by an event or injury in service (such as wearing of combat boots or a foot injury) then service-connection can be established based on pre-service aggravation.
If it was not noted on enlistment (38 CFR 3.304(b))
If a disability was not noted on your enlistment examination, then the tables turn – the burden is on VA to prove that the disability pre-existed service and that it was NOT aggravated beyond natural progression by your military service. i.e. VA must rebut the presumption of soundness in order to deny.
If they cannot prove this, then the presumption of soundness is not rebutted and VA must presume that you were sound on enlistment. However, this does not mean that your claim is automatically granted.
All it means is that VA will ignore the evidence showing that your evidence pre-existed service. They will then work your claim as a claim for direct service-connection, because they are presuming that you were sound on enlistment. It’s as if you did not have a pre-existing disability.
Because VA is not assuming that you were sound on enlistment, a grant of service connection must be based on direct service connection (or possibly presumptive service-connection in special circumstances).
A denial under this law would be based on a VA determination that the evidence clearly and unmistakably shows that your disability pre-existed service and was not aggravated by service. Because a denial means the presumption of soundness is rebutted, a denial of service connection under this law will be similar to the denial for a condition that was noted on enlistment – it will state that your condition was found to have pre-existed service and was not aggravated beyond natural progression.
An example would be sinusitis noted during childhood. If sinusitis is NOT noted on the enlistment examination, but the enlistment exam does note that the veteran had a history of sinusitis from ages 8-10, with no symptoms noted since. However, during service the veteran was treated for sinusitis.
What happens here is that VA will request a pre-service aggravation opinion. If the opinion states that the condition was aggravated beyond natural progression by service, it doesn’t mean they can grant it. All it means is that the presumption of soundness is not rebutted. The VA must then request a direct medical opinion if the current asthma is caused by the asthma during service. They will direct the examiner to ignore the sinusitis treated from ages 8-10 and instruct the examiner to assume that the veteran was sound on enlistment and did not have sinusitis prior to service.
If, however, the opinion states that the condition was not aggravated beyond natural progression by service, then the presumption of soundness is rebutted. The VA can then deny service connection for asthma by stating that it pre-existed service and that it was not aggravated beyond natural progression by service.
1151 Claims (Disabilities caused by VA Care)
Under this law, if a veteran suffers an additional disability or death due to VA medical treatment, hospitalization, or examination, and it resulted from negligence, carelessness, lack of skill, error in judgment, or an event not reasonably foreseeable, the veteran is entitled to compensation as if service-connected.
So, unlike all other forms of service-connection, claims under this law do not require an in-service event. It is also perhaps important to note that VA does not call this service-connection. It is simply called “compensation under 38 USC 1151”, after the law on which it is based.
It sounds pretty straightforward, but there are a lot of things to consider here.
The most important is that VA hospital care, medical or surgical treatment, or examination must be furnished
- By a VA employee, and/or
- In a VA facility
That is a pretty big caveat. Basically, what qualifies as a VA employee and a VA facility is defined in 38 CFR 3.361.
It eliminates a lot of things. VA contract examinations, such as those handled by outside contractors like QTC and VES are not considered to be done by VA employees or to have been done in a VA facility.
Nursing home care or hospital care furnished outside of VA, even if contracted by VA, also do not count.
Additional disability incurred as a result of a medical procedure conducted by a non-VA employee in a non-VA facility even if a VA physician had provided advice or recommendation for this procedure is also not covered. Basically, the courts have ruled that merely authorizing or paying for care at a private facility does not make it VA care.
“Not Reasonably Foreseeable” Events
To qualify under this category, the additional disability must not be a known or expected complication of the procedure.
It must be something that a reasonable health care provider would not have anticipated as an ordinary risk of treatment.




Pingback: What is Toxic Exposure Risk Activity (TERA)? – VetHacker